Introduction
Alaska occupies an outsized place in the American imagination: vast, remote, and rich in natural resources. Yet that same geography that defines the state also shapes its social institutions — especially health care. The question of who receives timely, culturally appropriate, and effective health services in Alaska is not merely a matter of hospital location or insurance coverage. It is a story about colonial history, the social determinants of health, infrastructural politics, and the adaptive strategies of Indigenous and rural communities.
This article examines healthcare access and inequality in Alaska from a sociological perspective: mapping structural barriers, analyzing the role of institutions and social networks, and suggesting policy and community-grounded pathways for reducing inequities.

Structural and geographic determinants of access
Alaska’s geography is extreme: more than 80% of the state lacks connection to the continental road system, and many communities are reachable only by air or seasonal water routes. This physical isolation multiplies the usual barriers to care: long travel times, high costs of transport, and limited availability of specialists. Emergency care frequently requires medevac flights, and routine referrals—say to a cardiologist or oncologist—often force residents to make time-consuming, expensive journeys to regional hubs. The result is delayed care, higher out-of-pocket expenses, and an overreliance on emergency services for conditions that could be managed earlier in primary care.
From a sociological vantage, these geographic constraints produce what patients experience as “distance-based” marginality: not just physical separation from providers but a chronic uncertainty about whether help will arrive in time. Distance affects social relations too—families may be torn when a patient must relocate for long treatment regimens; social supports fray; and the social capital of small communities is redirected into caregiving and transport logistics rather than prevention or health promotion. Rurality in Alaska is therefore not only spatial but deeply social.
Historical and institutional contexts: colonial legacies and tribal health systems
Health inequalities in Alaska cannot be separated from the longer history of colonization, dispossession, and federal-state policy toward Indigenous peoples. Alaska Native communities experienced epidemics, forced relocations, boarding schools, and systemic neglect — historical traumas that continue to shape trust in institutions and patterns of morbidity today. These structural injustices contribute to elevated rates of chronic disease, mental health challenges, substance use disorders, and mortality in many Alaska Native populations.
At the same time, Indigenous-led institutions have developed resilient responses. Tribal health organizations and networks play a central role in providing culturally grounded services and in negotiating with federal and state agencies. One notable institutional innovation is the statewide Community Health Aide/Practitioner (CHA/P) network, which places trained community health workers in remote villages to provide frontline care, triage, and continuity with larger hospitals. This program grew from a pragmatic response to epidemics and now forms part of the safety net for rural Alaska.
Another key institutional actor is the Alaska Native Tribal Health Consortium, which coordinates specialty services, training, and public health programs tailored to Alaska Native communities. Such organizations illustrate a dual dynamic: Indigenous communities are simultaneously disproportionately harmed by structural inequality and essential actors in community-rooted solutions.
Health outcomes and disparities: who is disadvantaged?
Statistically, American Indian and Alaska Native (AI/AN) populations face considerable disparities in health outcomes compared to national averages: higher prevalence of diabetes, certain infectious diseases, and injuries; poorer maternal and child health metrics in some regions; and disproportionate rates of substance-use related mortality. These disparities are shaped by poverty, housing instability, food insecurity, lower access to specialty care, and constrained behavioral health resources.
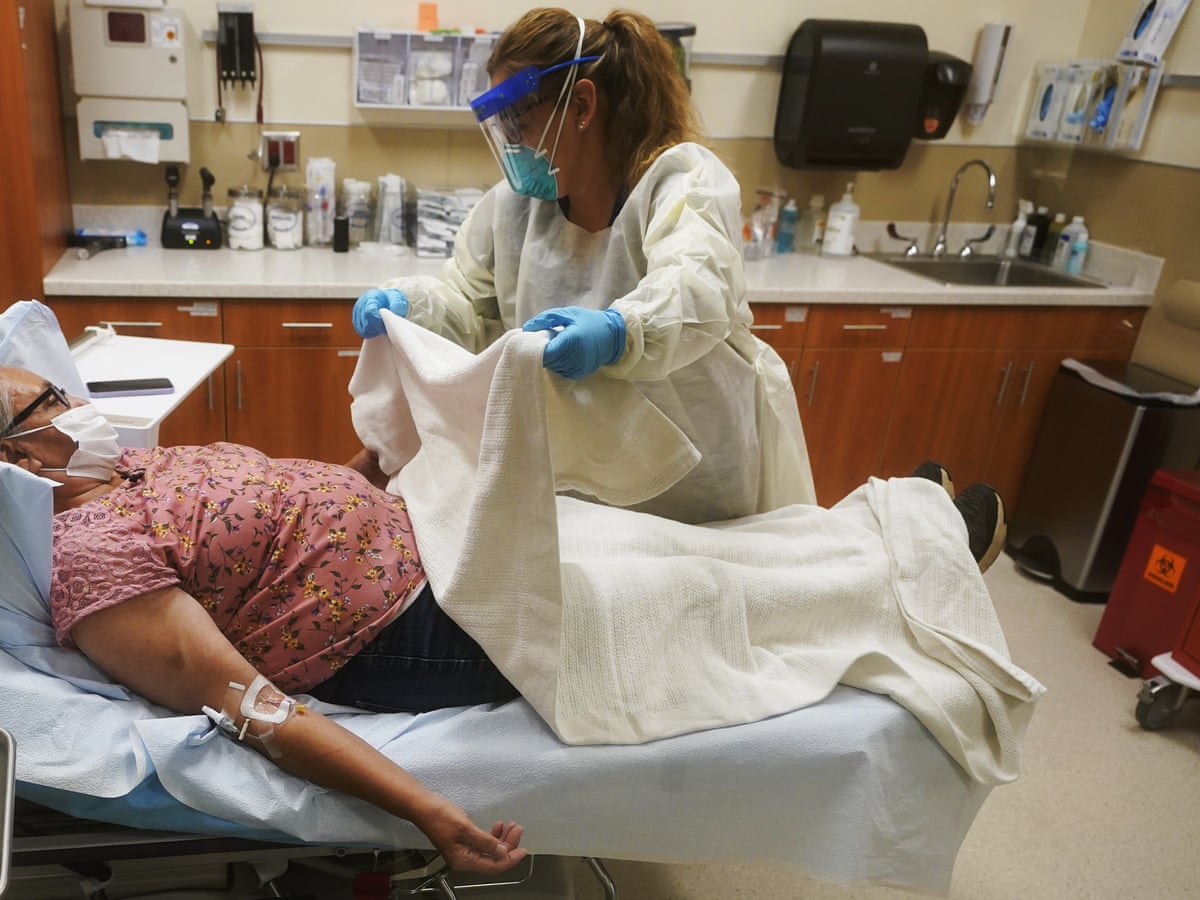
But the patterns are uneven. Urban Alaska Natives in Anchorage may have different service access than remote villagers relying on CHA/Ps; meanwhile non-Indigenous rural residents also experience barriers, especially those of lower socioeconomic status. A sociological lens foregrounds intersectionality: race/ethnicity, class, geography, age, and disability interact to produce variegated vulnerabilities across the state. Public health surveillance and qualitative studies both show that coverage rates alone do not predict service use—having insurance does not guarantee local providers, culturally safe care, or timely referrals.
The paradox of coverage vs. access
At the national level, debates about “coverage” (insurance) sometimes obscure “access” (ability to use care effectively). In Alaska, this paradox is visible: Medicaid and Indian Health Service (IHS) programs provide coverage for many residents, including a substantial share of Alaska Native people. Yet the mere presence of insurance does not eliminate the barriers of travel cost, provider shortages, cultural dissonance, or structural stigma. For instance, a patient with Medicaid in a remote village may still need to fly to a regional center and incur lodging and lost-wage costs—burdens not captured in coverage statistics.
Sociologists describe this mismatch using the concept of “structural adequacy”: institutions (like insurance) may exist but be inadequate given the social and material environment. Consequently, policy debates must move beyond enrollment numbers toward investments in logistics, local workforce development, and culturally responsive services.
Workforce shortages and the role of mid-level and community providers
Like many rural regions, Alaska faces shortages of physicians and specialists. To fill the gap, Alaska has leaned on mid-level providers (nurse practitioners, physician assistants), community health aides/practitioners, and telemedicine. The CHA/P system is a paradigmatic example: local residents receive training and certification to provide a breadth of primary care, behavioral health first response, and emergency stabilization. Because CHA/Ps are embedded in their communities, they bring social knowledge, language competency, and trust—qualities that reduce friction in care-seeking and increase preventive counseling effectiveness.
From a sociological perspective, CHA/Ps reconfigure professional boundaries and decentralize care, shifting the center of clinical authority into the village. This has implications for power, identity, and the moral economy of health: it valorizes local expertise while sometimes exposing CHA/Ps to ethical dilemmas when specialized referrals are unavailable. Strengthening these roles, formalizing career pathways, and ensuring adequate supervision and support are crucial policy measures.
Telehealth: promise and limits
Telehealth has been heralded as a technological fix to Alaska’s distance problem. During the COVID-19 pandemic, telemedicine expanded rapidly, offering remote consultations, mental health counseling, and follow-up care without travel. For many patients, telehealth reduced the time and costs of accessing a specialist.

However, telehealth is not a panacea. Reliable broadband remains uneven across the state; digital literacy varies; and some clinical encounters (physical exams, certain diagnostics) cannot be fully substituted by virtual care. Additionally, sociocultural dynamics matter: patients may prefer face-to-face encounters, seek care in languages other than English, or have privacy concerns in small homes where confidential tele-sessions are difficult. Telehealth therefore improves access for some while leaving others behind, potentially deepening inequalities if not paired with investments in infrastructure and digital inclusion.
Mental health, substance use, and social suffering
Alaska’s data show concerning trends in mental health and substance use, including elevated suicide and overdose rates in specific populations and regions. These outcomes are shaped by social determinants such as historical trauma, economic marginalization, social isolation, and limited behavioral health capacity. The state’s remote geographies exacerbate social suffering: when community members cannot access counseling, group supports, or ongoing addiction treatment, cycles of trauma and substance dependence intensify.
Effective responses must be socio-structural: expanding mobile crisis teams, funding culturally competent behavioral health programs, integrating traditional healing practices with clinical care, and addressing upstream determinants like housing and employment. Community-led harm-reduction efforts have emerged in some towns, demonstrating the power of local social capital in the absence of adequate formal services.
Economic and policy drivers: cost, funding, and political choices
Delivering health care in Alaska is expensive. Transportation of supplies and personnel, heating and facility maintenance, and medevac logistics inflate per-capita costs. These economic realities intersect with political choices: state budget allocations, Medicaid reimbursement rates, funding for tribal health organizations, and federal support for rural programs determine what services remain viable.
Policy decisions that treat Alaska’s health system as though it were a smaller version of the Lower 48 miss its distinctiveness. Effective policy requires tailored financing—higher reimbursement for rural providers, subsidies for patient travel, and long-term investment in local workforce pipelines. Importantly, sovereignty and partnership with tribal governments must be center-stage: tribal organizations often administer health services effectively, but they need predictable and flexible funding to innovate.
Social networks, reciprocity, and community resilience
While structural deficits are profound, local communities exhibit resilience built on dense social networks and reciprocal practices. Families, neighbors, and tribal institutions often mobilize transport, caregiving, and informal counseling—acts that mitigate acute crises. For sociologists, these practices are not just stopgaps but evidence of social capital: norms of mutual aid, trust, and collective responsibility that sustain health in adverse conditions.
Policy should support such community resources rather than supplant them. Training programs, microgrants for community health projects, and formal partnerships that respect local leadership can amplify these strengths without erasing local autonomy.
Cultural competence and patient-centered care
Inequalities are aggravated when health services ignore cultural differences. Language barriers, varying belief systems about illness, and historical mistrust reduce the effectiveness of standard clinical encounters. Culturally competent care—delivered in local languages, integrating traditional healing practices, and recognizing the social meanings of illness—improves uptake and outcomes.
Sociological research underscores that cultural competence is relational: it requires genuine engagement, long-term relationships, and institutional humility. Training clinicians in cultural humility, recruiting staff from local communities, and co-designing services with tribal elders can bridge gaps in trust.
Recommendations — toward equitable health access in Alaska
Below are sociologically informed recommendations that combine structural, institutional, and community-level interventions:
- Invest in local workforce pipelines. Expand training, certification, and career ladders for CHA/Ps, mid-level providers, and behavioral health practitioners drawn from local communities. Financial incentives and distance-learning pathways can increase retention.
- Boost transportation and lodging supports. Create predictable travel subsidies for patients needing specialist care, and fund patient lodging near referral centers to reduce the economic burden on families.
- Strengthen tribal–state partnerships. Increase flexible funding to tribal health organizations, support co-governance of health programs, and recognize tribal sovereignty in program design.
- Expand broadband and digital inclusion. Pair telehealth expansion with investments in broadband infrastructure and digital literacy programs, ensuring telemedicine benefits are equitably distributed.
- Scale culturally grounded behavioral health programs. Support integration of traditional healing and community-based mental health services with clinical care to address substance use and suicide prevention.
- Adopt equity-focused monitoring. Use data systems that disaggregate outcomes by race, geography, and income to identify hotspots of inequity and evaluate interventions.
- Support community-led harm reduction. Fund grassroots harm-reduction and peer-led recovery initiatives that are often first responders in overdose crises.
These recommendations emphasize the interplay of material investment and sociocultural respect: building systems that are both technically adequate and socially legitimate.
Conclusion
Healthcare access and inequality in Alaska are products of geography, history, policy, and community dynamics. The state’s remoteness, colonial legacies, and economic constraints have generated distinctive challenges—but Alaska’s Indigenous institutions, community health aides, and localized social networks also offer powerful models of resilience and innovation. Addressing inequities requires more than funding clinics: it demands structural rethinking (transport, workforce, and financing), genuine partnership with tribal actors, and a commitment to culturally anchored care. A sociological approach underscores that health is made and remade in societal relationships; to improve outcomes in Alaska, policy must reshape those relationships toward justice, dignity, and local empowerment.
Selected sources & further reading
- CDC — Health Disparities in American Indian & Alaska Native populations.
- Alaska Native Tribal Health Consortium — Health aide training and services.
- BMJ/EMJ reporting on medevac and emergency care geography in Alaska.
- Rural Health Information Hub — Rural healthcare access overview and evidence.
Do you like this this Article ? You Can follow as on :-
Facebook – https://www.facebook.com/hubsociology
Whatsapp Channel – https://whatsapp.com/channel/0029Vb6D8vGKWEKpJpu5QP0O
Gmail – hubsociology@gmail.com
FAQs
1. What does Inequality in Alaska mean in the context of healthcare?
Inequality in Alaska refers to unequal access to healthcare services based on geography, race, income, and infrastructure. Remote villages, Indigenous communities, and low-income residents often face greater barriers than urban populations.
2. How does geography contribute to Inequality in Alaska?
Alaska’s vast and isolated terrain makes transportation difficult. Many communities are accessible only by air or boat, increasing the cost and time required to access medical care, which deepens Inequality in Alaska.
3. Who is most affected by Inequality in Alaska?
Alaska Native communities, low-income rural residents, elderly populations, and people with chronic illnesses are disproportionately affected by Inequality in Alaska.
4. How does rural living increase Inequality in Alaska?
Rural residents often lack nearby hospitals, specialists, and mental health providers. Travel for treatment may require expensive flights, making healthcare access uneven and reinforcing Inequality in Alaska.
5. What role does income play in Inequality in Alaska?
Lower-income households struggle with travel costs, medication expenses, and lost wages due to medical trips, contributing significantly to Inequality in Alaska.
6. How does workforce shortage impact Inequality in Alaska?
Limited availability of doctors, specialists, and mental health professionals in remote regions increases wait times and reduces quality of care, worsening Inequality in Alaska.
7. Can telehealth reduce Inequality in Alaska?
Telehealth has improved access for some communities, but limited broadband connectivity and digital literacy gaps mean it does not fully eliminate Inequality in Alaska.
8. How does historical marginalization influence Inequality in Alaska?
Colonial legacies and historical trauma among Indigenous populations contribute to mistrust in institutions and long-term health disparities, intensifying Inequality in Alaska.
9. What is the connection between mental health and Inequality in Alaska?
Higher rates of suicide, substance use disorders, and limited behavioral health services highlight how mental health challenges are deeply tied to Inequality in Alaska.
10. Does insurance coverage eliminate Inequality in Alaska?
No. Even with Medicaid or public health coverage, transportation barriers and lack of nearby providers mean Inequality in Alaska persists beyond insurance status.
11. How does climate affect Inequality in Alaska?
Harsh winters, extreme cold, and weather-related disruptions can delay medical transport and supply delivery, contributing to Inequality in Alaska.
12. What role do community health aides play in addressing Inequality in Alaska?
Community-based health workers improve local access and culturally sensitive care, helping reduce—but not fully eliminate—Inequality in Alaska.
13. How does food insecurity relate to Inequality in Alaska?
High food costs and limited fresh produce in remote areas contribute to chronic illnesses like diabetes, reinforcing health-related Inequality in Alaska.
14. What policies can reduce Inequality in Alaska?
Investing in rural infrastructure, expanding workforce training, supporting tribal health systems, and improving transportation subsidies can significantly reduce Inequality in Alaska.
15. Why is Inequality in Alaska a sociological issue?
Inequality in Alaska is shaped by social structures—class, race, geography, and policy decisions—making it not only a medical concern but also a broader issue of social justice and systemic inequality.
